IUI Process Explained Step by Step
Have you been trying to conceive for some time and your doctor has recently suggested IUI as the next step? Perhaps you agreed during the consultation, noted it down, and later searched to understand...
Have you been trying to conceive for some time and your doctor has recently suggested IUI as the next step?
Table Of Content
- Who is IUI Recommended For?
- Who Should Not Choose IUI?
- IUI Process Step by Step — Complete Walkthrough
- Step 1 — Initial Consultation and Investigation
- Step 2 — Deciding Between Natural and Stimulated IUI
- Step 3 — Monitoring the Cycle with Ultrasound
- Step 4 — Trigger Injection
- Step 5 — Sperm Collection and Preparation
- Step 6 — The IUI Procedure Itself
- Step 7 — Post-IUI Medications
- Step 8 — The Two-Week Wait and Pregnancy Test
- Natural IUI vs Stimulated IUI — What is the Difference?
- What Happens on the Day of IUI?
- Success Rates of IUI in India
- What affects IUI success rates
- How Many IUI Cycles Should You Try?
- Side Effects and Risks of IUI
- Emotional Side of the IUI Journey
- What to Do After IUI — The Two-Week Wait
- What Happens if IUI Fails?
- Lifestyle Tips to Improve IUI Success
- Questions to Ask Your Fertility Doctor Before IUI
- Warning Signs You Need a Fertility Specialist Now
- Frequently Asked Questions
- Dr Curo is With You Every Step
Perhaps you agreed during the consultation, noted it down, and later searched to understand what it really involves, including questions around IUI treatment cost India. You might be feeling a mix of hope and uncertainty wondering if this is the right option for you and whether it will be successful.
Whatever brought you here, you are in the right place.
IUI (Intrauterine Insemination) is one of the most commonly recommended fertility treatments in India. It is less complex than IVF, minimally invasive, more affordable, and for the right candidates, quite effective.
And like most medical procedures, it becomes far less intimidating once you understand it clearly step by step, in simple terms.
Who is IUI Recommended For?
IUI works best in specific situations. Here is who typically benefits most:
Unexplained infertility — When all tests come back normal but pregnancy has not happened after a year or more of trying, IUI is a reasonable and well-supported first treatment step.
Mild male factor infertility — Slightly low sperm count, mildly reduced motility, or minor morphology issues. IUI compensates by placing a concentrated, prepared sample of the best sperm directly inside the uterus.
Cervical factor infertility — When the cervical mucus is too thick or hostile to sperm preventing sperm from passing through — IUI bypasses the cervix entirely.
Ovulation disorders — Women with irregular ovulation due to PCOS or other hormonal issues can use IUI alongside ovulation-stimulating medicines to time the procedure accurately.
Single women or same-sex couples using donor sperm — IUI is the standard, minimally invasive method for conception using donor sperm.
Sexual dysfunction — When physical conditions prevent natural intercourse but both partners are otherwise fertile, IUI provides an effective alternative route.
Mild endometriosis — In mild cases where the tubes are still open and sperm and egg quality are good, IUI can be effective.
Who Should Not Choose IUI?
IUI is not appropriate for everyone. Your doctor will advise against it in these situations:
- Both fallopian tubes are blocked sperm cannot reach the egg even if placed in the uterus
- Severe male factor infertility very low sperm count, very poor motility, or very high abnormal forms where even the best prepared sample is unlikely to achieve fertilisation
- Severe endometriosis affecting tubal function
- Significant uterine abnormalities like large fibroids or severe adhesions that would prevent implantation
- Diminished ovarian reserve when egg quantity and quality are very low, more aggressive treatment like IVF gives a better chance
- Previous multiple failed IUI cycles if three to six IUI cycles have not worked, moving to IVF is typically the right next step
Understanding who IUI is and is not suited for is just as important as understanding the procedure itself. At Dr Curo, the fertility specialists we work with are honest about this from the very first consultation.
IUI Process Step by Step — Complete Walkthrough
Here is the complete IUI process step by step from your first appointment to the pregnancy test.
Step 1 — Initial Consultation and Investigation
Before IUI can be planned, both partners undergo a thorough fertility evaluation.
For the woman:
- Blood tests to check hormone levels — FSH, LH, AMH, prolactin, thyroid
- Pelvic ultrasound to assess the uterus, ovaries, and ovarian reserve
- Hysterosalpingography (HSG) —an X-ray test to confirm that at least one fallopian tube is open and functional. This is essential IUI cannot work if both tubes are blocked
For the man:
- Semen analysis evaluating sperm count, motility, morphology, and volume
- If the semen analysis result is borderline or abnormal, a repeat test is usually requested before making decisions
Once all results are available, your fertility specialist reviews them together and decides whether IUI is appropriate and whether natural or stimulated IUI is better for your situation.
This step typically takes one to two weeks.
Step 2 — Deciding Between Natural and Stimulated IUI
There are two ways to approach IUI. Your doctor will recommend one based on your investigations.
Natural cycle IUI — No medications are used. The procedure is timed around your natural ovulation. This is simpler and involves fewer side effects but is only appropriate when you ovulate regularly on your own.
Stimulated IUI — Low-dose fertility medicines are used to stimulate the ovaries to produce one or two mature follicles, making ovulation more predictable and giving IUI a better chance. This is the more commonly recommended approach.
Medicines used in stimulated IUI include:
- Oral medicines — Clomiphene citrate (Clomid) or Letrozole tablets taken from Day 2 to Day 6 of the menstrual cycle. These are simple to take and well-tolerated by most women.
- Injectable gonadotropins — Low-dose FSH injections given for several days. These are more powerful than tablets and used when tablets alone do not produce adequate follicle growth.
Your doctor will choose the right medicine and dose based on your hormone levels, age, and ovarian reserve.
Step 3 — Monitoring the Cycle with Ultrasound
Once stimulation medicines are started, you will attend the clinic for follicle monitoring ultrasound scans typically two to three times during the cycle.
These scans track the growth of follicles in the ovaries. A follicle is the fluid-filled sac that contains a maturing egg. When a follicle reaches approximately 18 to 22 millimetres in size, the egg inside is considered mature and ready for ovulation.
Monitoring is important for two reasons:
First to time the IUI procedure accurately. The procedure must be done within 24 to 36 hours of ovulation for the best chance of success.
Second to ensure stimulation has not been excessive. If too many follicles develop, the cycle may be cancelled to avoid the risk of a high-order multiple pregnancy.
Blood tests to check oestrogen and LH levels may also be done alongside ultrasounds.
This monitoring phase usually spans Day 8 to Day 14 of the cycle, depending on when follicles mature.
Step 4 — Trigger Injection
When monitoring confirms that one or two follicles are mature and ready, your doctor will instruct you to take a trigger injection usually an HCG injection or a GnRH agonist trigger.
This injection precisely triggers the final stage of egg maturation and causes ovulation to occur within 36 to 40 hours.
The timing of this injection is critical. Your clinic will tell you exactly what time to give the injection and your IUI will be scheduled accordingly, usually 36 to 40 hours later.
The trigger injection is given subcutaneously just under the skin and can be self-administered at home after simple instruction. Most women find it very manageable.
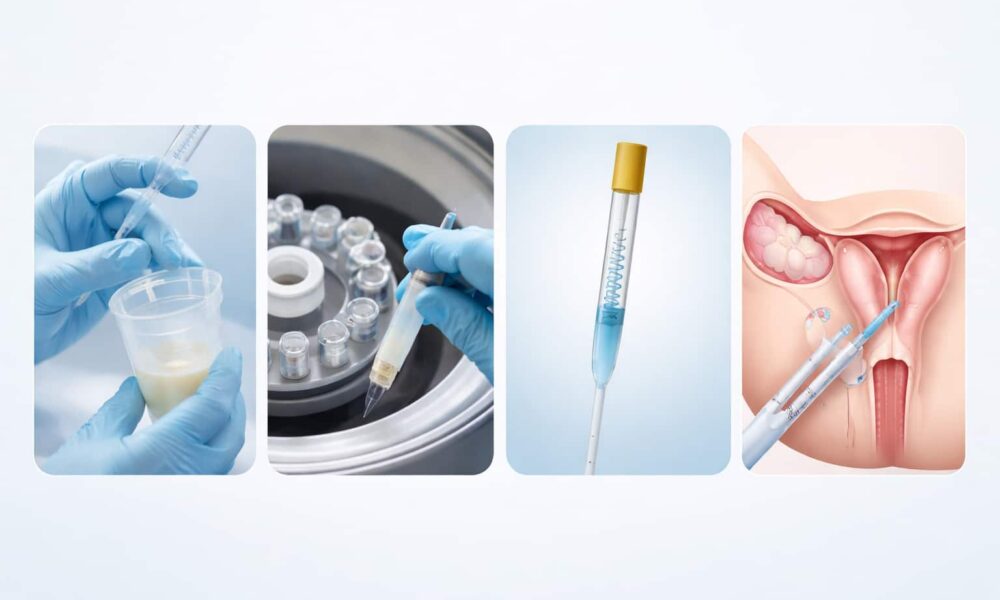
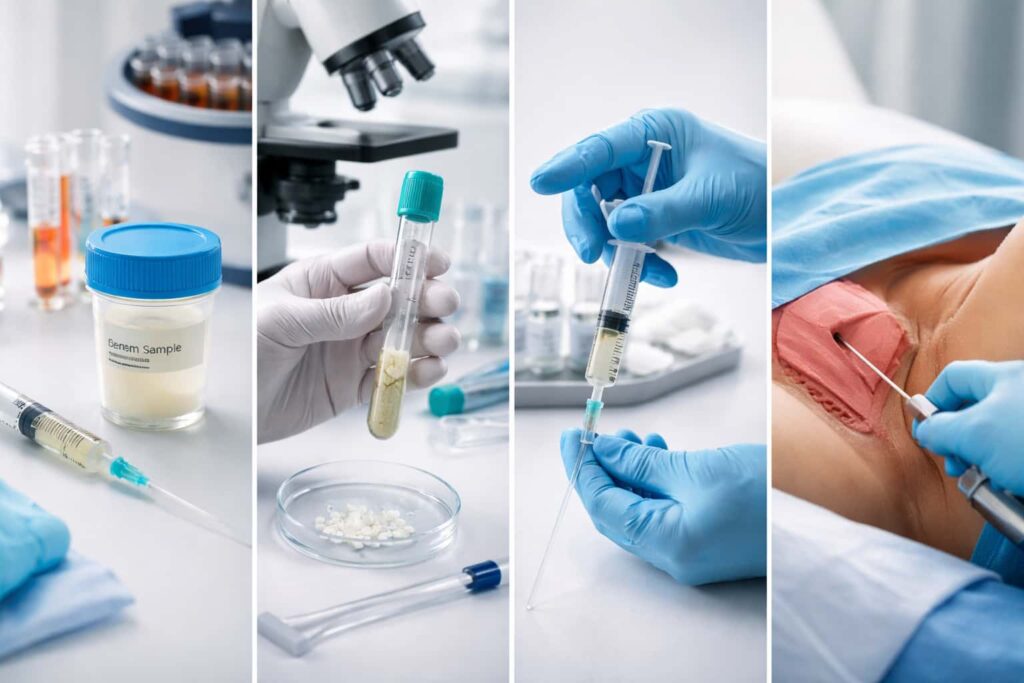
Step 5 — Sperm Collection and Preparation
On the morning of the IUI procedure usually 36 hours after the trigger injection the male partner provides a semen sample at the clinic by ejaculation into a sterile collection cup.
If sperm are being frozen or donor sperm is being used, the sample is thawed and prepared on the same morning.
The sample then goes to the laboratory for a process called sperm washing one of the most important steps in the entire IUI process.
What sperm washing involves:
The raw semen sample contains not just sperm but also seminal fluid, dead sperm, debris, white blood cells, and prostaglandins substances that would cause severe cramping if placed directly into the uterus.
Sperm washing removes all of this and concentrates the best, most motile sperm into a small volume of clean solution typically 0.3 to 0.5 millilitres. This concentrated, pure sample is what gets placed into the uterus.
The washing process takes approximately 45 minutes to one hour. Common techniques include density gradient centrifugation and swim-up preparation both designed to select the strongest, healthiest sperm.
After washing, the sample is analysed to confirm total motile sperm count. A minimum of 5 million motile sperm in the prepared sample is generally considered the threshold for IUI to be worthwhile.
Step 6 — The IUI Procedure Itself
This is the step most couples feel most anxious about before it happens and the most relieved about once it is done.
The IUI procedure is simple, quick, and for most women, causes minimal discomfort.
Here is exactly what happens:
You lie on the examination table as you would for a routine gynaecological exam. Your doctor inserts a speculum into the vagina to visualise the cervix — exactly as in a Pap smear.
A very thin, flexible catheter a soft tube is gently passed through the cervix into the uterine cavity. Most women feel mild pressure or a brief cramp at this point. Some feel nothing at all.
The prepared sperm sample is slowly injected through the catheter directly into the uterus. The catheter is then gently removed.
The entire procedure from start to finish takes approximately five to ten minutes.
You are then asked to rest on the table for 10 to 15 minutes before getting up. After that you can go home. There is no need for bed rest, hospitalisation, or any special precautions for the rest of the day. Many women go back to work the same day.
Step 7 — Post-IUI Medications
After the procedure, your doctor will typically prescribe progesterone support usually as vaginal pessaries or oral tablets to help prepare and maintain the uterine lining for potential implantation.
Progesterone is the hormone that the body produces naturally after ovulation to support early pregnancy. Supplementing it after IUI is common practice and helps create the best possible environment for an embryo to implant.
You will take progesterone support daily until the pregnancy test and if the test is positive, usually until the 10th to 12th week of pregnancy.
Step 8 — The Two-Week Wait and Pregnancy Test
After the IUI procedure, you wait approximately 14 days before taking a pregnancy test. This is the time needed for a fertilised egg to implant, begin developing, and produce enough HCG hormone to be detected.
A blood test called a serum beta HCG test is more sensitive than a urine test and is the preferred way to confirm pregnancy after IUI.
If the result is positive your fertility specialist will arrange an early ultrasound at around 6 to 7 weeks to confirm a healthy intrauterine pregnancy.
If the result is negative your specialist will review the cycle, discuss what can be adjusted, and plan whether to proceed with another IUI cycle or consider other options.
Natural IUI vs Stimulated IUI — What is the Difference?
| Factor | Natural IUI | Stimulated IUI |
| Medicines used | None | Yes — tablets or injections |
| Monitoring scans needed | One or two | Two to three |
| Ovulation predictability | Depends on natural cycle | More controlled and predictable |
| Number of eggs | One | Usually one to two |
| Success rate per cycle | Slightly lower | Slightly higher |
| Side effects | Minimal | Mild bloating, mood changes possible |
| Cost | Lower | Slightly higher due to medicines |
| Best for | Regular ovulators, normal hormones | PCOS, irregular ovulation, borderline sperm |
Most fertility specialists in India recommend stimulated IUI because the slightly better success rate per cycle makes the overall treatment journey shorter and more productive.
What Happens on the Day of IUI?
Many couples find it helpful to know exactly what the day looks like. Here is a realistic picture:
Morning — The male partner produces the semen sample at the clinic, usually between 7 and 9 am. The sample goes to the laboratory immediately for sperm washing.
45 to 60 minutes later — The laboratory confirms the prepared sperm count and quality. The clinic schedules your procedure time.
Procedure time — You go into the procedure room. The IUI itself takes five to ten minutes. You rest for 10 to 15 minutes afterwards.
After the procedure — You can eat, drink, and go about your day normally. Mild cramping similar to period pain is common for a few hours and is completely normal. Light spotting occasionally occurs also normal.
What to avoid on the day — Heavy exercise and sexual intercourse on the day of IUI itself. Your doctor will advise when these can be resumed.
Medicines — Take your prescribed progesterone support as instructed from the evening of the procedure day.
There is no drama. No crisis moments. Most couples describe it as far simpler than they expected.
Success Rates of IUI in India
Understanding IUI success rates honestly without false hope and without unnecessary pessimism is important.
| Age Group | Success Rate per IUI Cycle |
| Under 30 years | 18 to 25 percent |
| 30 to 34 years | 15 to 20 percent |
| 35 to 37 years | 10 to 15 percent |
| 38 to 40 years | 8 to 12 percent |
| Above 40 years | 5 to 8 percent |
What affects IUI success rates:
- Woman’s age — the single most influential factor
- Cause of infertility — IUI works best for cervical factor, mild male factor, and unexplained infertility
- Sperm quality after washing — higher motile sperm count in the prepared sample improves outcomes
- Number of mature follicles — one or two gives a better chance than just one alone
- Uterine and tubal health
- Timing accuracy — IUI done too early or too late relative to ovulation reduces success significantly
- Stimulated vs natural cycle — stimulated cycles generally perform better
Cumulative success rates across multiple cycles are much more encouraging:
- After 3 IUI cycles — approximately 30 to 40 percent cumulative pregnancy rate
- After 6 IUI cycles — approximately 50 to 60 percent cumulative pregnancy rate for suitable candidates
At Dr Curo, the fertility specialists we connect you with are honest about what IUI can realistically achieve for your specific situation so you can plan with clarity.
How Many IUI Cycles Should You Try?
This is one of the most common and most important questions couples ask.
Most fertility specialists recommend trying IUI for three to six cycles before considering moving to IVF — provided the diagnosis makes IUI appropriate.
Here is why:
Each IUI cycle is independent. A failed cycle does not reduce your chances in the next cycle. Cumulative success rates build meaningfully across multiple attempts.
However, after three to four failed IUI cycles, your specialist should review everything carefully because continuing IUI indefinitely without reassessment is not in your best interest.
Reasons to move from IUI to IVF sooner:
- Age above 37 time matters more and IVF gives a better chance per cycle
- Sperm count significantly lower than expected after washing
- No pregnancy after three cycles in women with good ovarian reserve
- New findings on investigation a tube that appeared open on HSG showing signs of poor function
The decision to continue IUI or move to IVF should always be made together with your fertility specialist based on your results, your age, and your emotional capacity for continued treatment.
Side Effects and Risks of IUI
IUI is one of the safest fertility procedures available. But being informed about possible side effects helps you feel prepared rather than alarmed.
Common and mild:
- Mild cramping during and after the procedure similar to period pain, usually resolving within a few hours
- Light spotting after the catheter is passed through the cervix completely normal and not a cause for concern
- Bloating and mild discomfort during the stimulation phase especially with injectable medicines
- Mood changes and emotional sensitivity a combination of hormones and the stress of the process itself

Less common:
- Ovarian Hyperstimulation Syndrome (OHSS) — occurs when the ovaries over-respond to stimulation medicines. Mild OHSS causes bloating and discomfort. Severe OHSS is rare with the low doses used in IUI. Your monitoring scans are specifically designed to catch signs of this early.
- Multiple pregnancy — if more than two mature follicles develop, there is an increased risk of twins or triplets. A cycle may be cancelled if too many follicles are seen on monitoring. This is why monitoring is not optional.
- Infection — extremely rare. The procedure is performed with sterile instruments and the risk of introducing infection is very low.
What IUI does not cause:
IUI does not damage the uterus, ovaries, or fallopian tubes. It does not reduce future fertility. It does not increase the risk of birth defects. It does not cause cancer.
At Dr Curo, every fertility specialist we work with explains side effects clearly before the procedure so nothing takes you by surprise.
Emotional Side of the IUI Journey
The medical side of IUI is straightforward. The emotional side is anything but.
Every couple going through IUI is carrying something heavy months or years of hoping, trying, wondering, and waiting. And now a treatment process that brings fresh hope alongside fresh anxiety about whether it will work.
Here is what many couples experience honestly:
The optimism of starting — Beginning IUI often feels like finally doing something. That feeling of action after months of uncertainty is genuinely comforting for most couples.
The anxiety of monitoring — Each scan becomes significant. Each follicle size feels important. The wait between appointments can feel very long.
The nervousness on procedure day — Even knowing the procedure is simple, many couples feel anxious. This is completely normal. Bring your partner if it helps. Ask the doctor to explain each step as it happens.
The weight of the two-week wait — This is almost universally described as the hardest part. Every twinge, every cramp, every early symptom or absence of symptoms gets analysed. Distraction helps. Rest helps. Talking to each other helps.
The grief of a negative result — A failed IUI cycle is a real loss. It deserves to be acknowledged as one. Give yourself time. Do not rush back into the next cycle before you are ready emotionally and not just physically.
What actually helps:
- Talking to each other honestly not protecting each other from your own fears
- Setting a clear limit in your mind for how many cycles you want to try before reassessing so you are not in an open-ended process
- Limiting how much you share with extended family and friends you control your own story
- Finding one or two people outside the process you can talk to freely
- Considering professional counselling fertility counsellors are trained specifically for this journey and are enormously helpful
At Dr Curo, emotional support is not an afterthought. We believe it is an essential part of fertility care.
What to Do After IUI — The Two-Week Wait
The period between the IUI procedure and the pregnancy test is medically called the luteal phase and informally called the two-week wait. Here is how to manage it well:
Take your medicines — Progesterone support is not optional. Take it exactly as prescribed, every day, without missing doses.
Live normally — There is no need for bed rest after IUI. Walking, working, cooking, socialising all of it is fine. Your uterus is not fragile. Normal life does not reduce your chances.
Avoid the following:
- Taking a pregnancy urine test before 14 days the trigger injection contains HCG and will give a false positive if tested too early
- Intense exercise or heavy lifting in the first few days post-procedure
- Alcohol throughout the two-week wait and ideally throughout treatment
- Smoking at all
Manage the anxiety practically:
- Plan something enjoyable for the middle of the two weeks a dinner, a short trip, a film something to look forward to that breaks the waiting
- Reduce searching symptoms online obsessively every symptom of early pregnancy also occurs in a non-pregnant cycle due to progesterone. You cannot tell from symptoms.
When to call your clinic:
- Severe cramping significantly worse than normal period pain
- Heavy bleeding before the test date
- Any symptom that genuinely worries you your clinic would rather you call than worry in silence
What Happens if IUI Fails?
A failed IUI cycle is disappointing. But it is not the end and it carries information that helps plan next steps.
What your fertility specialist will review:
- How many follicles developed and what size they were at trigger
- The sperm count and quality in the prepared sample
- Whether progesterone levels after the procedure were adequate
- Whether timing of the procedure was accurate
- Whether there are any new clinical findings to investigate
What might change in the next cycle:
- Adjusting stimulation medicine type or dose
- Changing the trigger timing
- Switching from oral medicines to injectables
- Investigating whether a factor was missed in the initial workup
When to consider moving to IVF:
- After three to four IUI cycles with no pregnancy in women under 35
- After two to three IUI cycles in women over 37 where time is more critical
- When new investigation reveals a factor that makes IUI unlikely to succeed
- When the emotional toll of continued IUI cycles is significant and IVF offers meaningfully better odds
Moving to IVF after failed IUI is not failure. It is intelligent, evidence-based decision making. At Dr Curo, your fertility specialist will guide this conversation with honesty and compassion never rushing you, and never keeping you in a treatment that is no longer your best option.
Lifestyle Tips to Improve IUI Success
The choices you make during a treatment cycle genuinely affect your outcomes. Here is what matters most:
Maintain a healthy weight — Both overweight and significantly underweight affect hormone balance, ovulation, and implantation. Even modest weight changes before treatment can improve outcomes meaningfully.
Quit smoking completely — Smoking damages egg quality, impairs sperm function, and reduces IUI success rates. Both partners should stop ideally at least three months before starting treatment.
Avoid alcohol — Even moderate alcohol consumption is associated with reduced fertility treatment success. Avoiding it entirely during treatment is the safest and most sensible approach.
Eat a balanced, nutrient-rich diet — A diet rich in vegetables, fruits, whole grains, lean proteins, and healthy fats supports hormonal health and egg quality. Reduce processed foods, sugar, and refined carbohydrates.
Take folic acid — Women trying to conceive should take 400 to 800 micrograms of folic acid daily starting before treatment begins and continuing into early pregnancy. This reduces the risk of neural tube defects significantly.
Manage stress actively — Extreme psychological stress affects hormone levels. Yoga, walking, meditation, and breathing exercises are all genuinely helpful not just nice to do. Choose what works for you and do it consistently.
Sleep well — Seven to eight hours of quality sleep every night supports hormone regulation, immune function, and emotional resilience during treatment.
Light exercise is beneficial — Walking, swimming, and gentle yoga are all positive during a treatment cycle. Intense, high-impact exercise should be avoided during stimulation and after the IUI procedure.
Limit caffeine — Keeping caffeine intake below 200 milligrams per day roughly one to two cups of coffee is the standard recommendation during fertility treatment.
Questions to Ask Your Fertility Doctor Before IUI
Going into your consultation fully prepared changes the entire experience. Here are the questions worth asking:
- Based on my investigations, is IUI a good option for us or would you recommend starting with IVF?
- Do you recommend natural or stimulated IUI in my case and why?
- Which stimulation medicine do you recommend tablets or injections?
- How many monitoring scans will I need during the cycle?
- What sperm count in the prepared sample would you consider adequate for IUI?
- How do you time the IUI precisely scan only, or blood test as well?
- What progesterone support will I take after the procedure?
- When exactly should I take the pregnancy test?
- How many IUI cycles would you recommend before reassessing?
- What is your clinic’s IUI success rate for my age group and diagnosis?
- What is the all-inclusive cost per cycle including medicines and scans?
A fertility doctor who answers these questions clearly and patiently is a doctor worth trusting with your care.
Warning Signs You Need a Fertility Specialist Now
Many couples wait far longer than they need to before seeking help. Here are the signs that it is time to consult a fertility specialist without further delay:
- You have been trying to conceive for 12 months or more and you are under 35
- You have been trying for 6 months or more and you are 35 or older
- You have very irregular periods or no periods at all
- You have been diagnosed with PCOS, endometriosis, or uterine fibroids
- You have had two or more miscarriages
- Your partner has been told his sperm count or quality is below normal
- You have had a pelvic infection, pelvic surgery, or an ectopic pregnancy in the past
- You are a single woman or same-sex couple planning to conceive using donor sperm
Seeking help early does not commit you to treatment. It gives you a full picture of where you stand and that information is genuinely powerful.
At Dr Curo, connecting with a verified fertility specialist is simple, confidential, and completely without pressure.
Frequently Asked Questions
Q1. What is the IUI process step by step in simple terms? The IUI process involves five main steps: taking medicines to stimulate ovulation, monitoring follicle growth with ultrasound, a trigger injection to time ovulation, sperm washing to prepare the sample, and finally placing the prepared sperm directly into the uterus through a thin catheter. After that, you wait two weeks before a pregnancy test.
Q2. Is IUI painful? Most women describe the procedure as feeling like mild period cramps brief and manageable. Some women feel nothing at all. It is not a surgical procedure and does not require anaesthesia. Most women go back to normal activity within a few hours.
Q3. How long does the entire IUI cycle take? One complete IUI cycle takes approximately three to four weeks from the start of your period to the pregnancy test.
Dr Curo is With You Every Step
The decision to begin fertility treatment is never easy. It takes real courage to accept that you need support, to trust a doctor with something so personal, and to continue through a process that can be both emotionally and physically demanding, especially when you are still trying to understand what is IUI treatment and whether it is right for you.
But one thing is certain: when you understand the IUI process step by step clearly and in simple language it becomes far less intimidating. And when fear reduces, you can focus on what truly matters: giving the treatment the best possible chance of success.
At Dr Curo, we focus on clarity and care. We do not rush consultations or overwhelm you with complex medical terms. Instead, we offer honest guidance, connect you with verified specialists, and provide ongoing support throughout your entire treatment journey not just at the start.
Dr Curo — Expert Care. The Right Doctor. A Healthier, Happier You.










No Comment! Be the first one.