Male Infertility Causes: What Every Man Should Know — Complete Guide
When a couple struggles to conceive, the focus often falls on the woman. But the truth is, in 40–50% of cases, the cause is linked to the male partner. At Dr Curo, we emphasize that male infertility...
When a couple struggles to conceive, the focus often falls on the woman. But the truth is, in 40–50% of cases, the cause is linked to the male partner.
Table Of Content
- What is Male Infertility?
- Why Talking About Male Infertility Matters
- Infertility Causes in Men — Complete Breakdown
- 1. Sperm Production Problems
- 2. Hormonal Imbalances
- 3. Varicocele
- 4. Blockages in the Reproductive Tract
- 5. Infections and STIs
- 6. Lifestyle Factors
- 7. Genetic Causes
- 8. Ejaculation Problems
- 9. Medications and Medical Treatments
- 10. Undescended Testes (Cryptorchidism)
- How is Male Infertility Diagnosed?
- Types of Male Infertility
- Treatment Options for Male Infertility at Dr Curo
- Success Rates — Can Male Infertility Be Treated?
- Cost of Male Infertility Treatment at Dr Curo
- Side Effects and Risks of Male Infertility Treatments
- Male Infertility and Emotional Wellbeing
- How Long Does Treatment Take?
- Tips to Improve Male Fertility Naturally
- Frequently Asked Questions
- Dr Curo is With You Every Step
At Dr Curo, we emphasize that male infertility is common, real, and often treatable. Understanding male infertility is a key step toward choosing the right infertility treatment India and avoiding delays.
This guide explains the causes of male infertility in simple, clear language to help couples take the right next step.
What is Male Infertility?
Male infertility is defined as the inability of a man to cause pregnancy in a fertile female partner after 12 months of regular, unprotected intercourse.
In most cases, male infertility comes down to one thing — a problem with the sperm. Either the sperm count is too low, the sperm are not moving correctly, their shape is abnormal, or there is a blockage preventing sperm from being delivered during ejaculation.
In simple terms for conception to happen naturally, a man needs to produce enough healthy, well-shaped, fast-moving sperm that can travel through the female reproductive tract and successfully fertilise an egg. When any part of that process is disrupted, infertility can result.
At Dr Curo, male infertility is evaluated thoroughly and treated with the same level of care and expertise as female infertility because both partners matter equally in this journey.
Why Talking About Male Infertility Matters
Male infertility is significantly underdiagnosed not because it is rare, but because it is underreported. Many men avoid getting tested due to embarrassment, cultural stigma, or the mistaken belief that fertility is primarily a female concern.
This silence has real consequences. Couples spend months or even years focusing exclusively on the woman going through hormone treatments, IUI cycles, and investigations when a simple semen analysis on the male partner could have identified the problem immediately and redirected treatment correctly from day one.
At Dr Curo, both partners are evaluated together from the very first consultation. This is not about blame it is about efficiency, accuracy, and giving every couple the fastest possible route to the family they want.

Infertility Causes in Men — Complete Breakdown
There are many different infertility causes in men. Here is a clear and thorough breakdown of the most common ones:
1. Sperm Production Problems
The most common category of male infertility involves issues with how sperm are produced in the testes.
Low sperm count (Oligospermia) — fewer than 15 million sperm per millilitre of semen. The lower the count, the harder it is for any sperm to reach and fertilise the egg naturally.
Zero sperm count (Azoospermia) — no sperm found in the ejaculate at all. This can be caused by a production failure in the testes or a blockage in the ducts that carry sperm out. This is one of the most treatable causes of male infertility with the right approach.
Poor sperm motility (Asthenospermia) — sperm that cannot swim properly or move in the right direction. Even with a normal count, poor motility means sperm cannot reach the egg.
Abnormal sperm shape (Teratospermia) — sperm with malformed heads, tails, or midpieces. Abnormally shaped sperm have difficulty penetrating the egg even if they reach it.
2. Hormonal Imbalances
The production of sperm is controlled by a hormonal chain that starts in the brain and ends in the testes. Problems at any point in this chain can reduce or stop sperm production entirely.
Key hormones involved include FSH (Follicle Stimulating Hormone), LH (Luteinising Hormone), and testosterone. When FSH or LH levels are too low a condition called hypogonadotropic hypogonadism the testes receive no signal to produce sperm. When testosterone is too low, sperm development is severely impaired.
Hormonal causes of male infertility are particularly important because they are often highly treatable with targeted hormone therapy and correcting the imbalance can restore natural sperm production in many cases.
3. Varicocele
A varicocele is an enlargement of the veins inside the scrotum similar to varicose veins in the legs. It is one of the most common and correctable infertility causes in men, found in approximately 15 percent of all men and in up to 40 percent of men being evaluated for infertility.
Varicoceles cause a rise in scrotal temperature and reduce blood flow to the testes. This disrupts sperm production, damages sperm DNA, and reduces sperm count and motility over time.
The good news varicocele repair through a minor surgical procedure or radiological intervention is highly effective. Many men see significant improvement in sperm parameters within 3 to 6 months of treatment.
4. Blockages in the Reproductive Tract
Even when the testes are producing sperm normally, a physical obstruction anywhere along the path from testes to ejaculation can prevent sperm from appearing in the semen. This is called obstructive azoospermia.
Common causes of blockages include:
- Previous infections particularly untreated chlamydia or gonorrhoea that caused scarring
- Previous vasectomy intentional surgical blockage of the vas deferens
- Congenital absence of the vas deferens some men are born without the tube that carries sperm, often associated with cystic fibrosis gene mutations
- Injury or trauma to the groin or reproductive tract
- Previous hernia repair surgery that inadvertently damaged the vas deferens
Blockages are diagnosed through clinical examination, ultrasound, and hormone tests. Surgical sperm retrieval techniques (TESA, PESA, microTESE) can recover sperm directly from the testes for use in IVF with ICSI even when blockages cannot be surgically corrected.
5. Infections and STIs
Certain infections directly damage sperm or block the reproductive tract through inflammation and scarring. The most significant include:
- Chlamydia and gonorrhoea — the most common STIs that cause reproductive tract damage in both men and women. Often completely symptom-free, meaning men carry them unknowingly for years
- Mumps orchitis — mumps infection after puberty can cause significant testicular inflammation, leading to permanent damage to sperm-producing cells in some cases
- Prostatitis and epididymitis — infection and inflammation of the prostate or epididymis disrupts sperm storage, maturation, and transport
- HIV and certain other viral infections — can affect sperm quality and hormone levels
Identifying and treating active infections is an essential part of any male fertility evaluation at Dr Curo.
6. Lifestyle Factors
This is the category with the most direct opportunity for positive change. Multiple everyday lifestyle choices have a measurable and significant impact on sperm quality.
Smoking — tobacco smoke contains toxins that damage sperm DNA, reduce sperm count, and impair motility. The effects are dose-dependent the more a man smokes, the greater the damage. Quitting smoking has been shown to meaningfully improve sperm parameters within 3 months.
Alcohol — heavy or regular alcohol consumption reduces testosterone levels, lowers sperm count, and increases the percentage of abnormally shaped sperm.
Heat exposure — the testes are located outside the body for a reason sperm production requires a temperature slightly below core body temperature. Hot baths, saunas, steam rooms, heated car seats, and even tight underwear raise scrotal temperature and reduce sperm production.
Obesity — excess body fat converts testosterone to oestrogen, disrupting the hormonal environment needed for healthy sperm production. Obese men have significantly higher rates of low sperm count and poor motility.
Stress — chronic psychological stress raises cortisol levels, which suppresses testosterone and disrupts the hormonal signals controlling sperm production.
Anabolic steroids and performance-enhancing drugs — one of the most dramatically damaging lifestyle choices for male fertility. Testosterone supplementation and anabolic steroids completely suppress the body’s natural hormone signals, shutting down sperm production entirely. In some cases this damage can be long-lasting or permanent.
Recreational drugs — marijuana, cocaine, and other recreational drugs all negatively affect sperm production, motility, and DNA integrity.
7. Genetic Causes
Some cases of male infertility have a genetic origin that cannot be changed but can be worked around with appropriate treatment.
Klinefelter syndrome — men born with two X chromosomes instead of one (XXY) typically have very low or no sperm production. Some may still have pockets of sperm in the testes that can be retrieved surgically.
Y chromosome microdeletions — small deletions in the Y chromosome can remove genes essential for sperm production. These deletions can be inherited by male children conceived through IVF and ICSI.
Cystic fibrosis gene mutations — men carrying two copies of the CFTR gene mutation are often born without the vas deferens, resulting in obstructive azoospermia.
Genetic testing is an important part of the evaluation for men with azoospermia or severely low sperm counts at Dr Curo.
8. Ejaculation Problems
Normal ejaculation is required for sperm to be delivered. Several conditions can disrupt this:
Retrograde ejaculation — sperm travels backward into the bladder instead of forward through the urethra during orgasm. Causes include diabetes, certain medications, and previous prostate or bladder surgery. Sperm can be retrieved from urine for use in IUI or IVF.
Premature ejaculation and ejaculatory dysfunction — can prevent normal intercourse but sperm can still be collected through other methods.
Erectile dysfunction — difficulty achieving or maintaining an erection prevents natural intercourse but does not affect sperm quality. Sperm can be collected through masturbation for fertility treatments.
Anejaculation — the complete absence of ejaculation, often neurological in cause, where sperm retrieval techniques can still recover viable sperm.
9. Medications and Medical Treatments
Several medications and medical treatments are known to damage sperm production sometimes temporarily, sometimes permanently.
- Chemotherapy and radiation — cancer treatments can severely and sometimes permanently damage sperm-producing cells. Sperm banking before treatment begins is strongly recommended for any man of reproductive age facing cancer treatment
- Sulfasalazine — used for inflammatory bowel disease, significantly reduces sperm count
- Certain antibiotics — notably nitrofurantoin
- Calcium channel blockers — used for blood pressure
- Antidepressants and antipsychotics — some affect hormone levels and ejaculation function
- Alpha-blockers — can cause retrograde ejaculation
Always inform your Dr Curo fertility specialist of every medication you are currently taking. Many effects are reversible once the medication is stopped or changed.
10. Undescended Testes (Cryptorchidism)
In some men, one or both testes failed to descend into the scrotum before birth. If left untreated during childhood, undescended testes lead to long-term damage to sperm-producing cells due to the higher internal body temperature. Even when surgically corrected in childhood, some degree of reduced fertility may remain in adulthood.
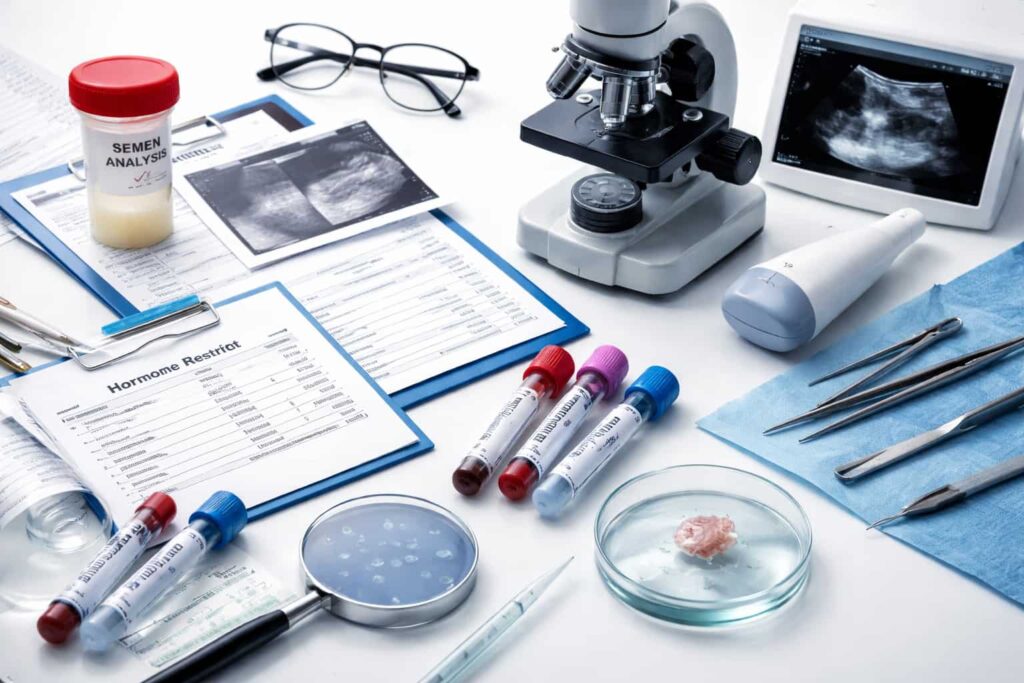
How is Male Infertility Diagnosed?
At Dr Curo, male infertility evaluation is structured, thorough, and non-invasive in the first instance.
Semen Analysis — the most important and foundational test. Evaluates sperm count, motility, morphology (shape), volume, pH, and the presence of white blood cells or infection. This single test provides enormous information and is always the starting point.
Hormone Blood Tests — FSH, LH, testosterone, prolactin, and thyroid function are measured to identify any hormonal cause of low sperm production.
Scrotal Ultrasound — checks for varicocele, testicular size and structure, and any abnormalities in the epididymis or vas deferens.
Genetic Testing — karyotype (chromosome analysis) and Y chromosome microdeletion testing for men with azoospermia or very low sperm counts.
Post-Ejaculation Urinalysis — checks for sperm in the urine to confirm or rule out retrograde ejaculation.
Testicular Biopsy — in selected cases of azoospermia, a small sample of testicular tissue is taken to determine whether sperm production is occurring inside the testes even when none appear in the ejaculate.
Types of Male Infertility
At Dr Curo, male infertility is broadly categorised to guide the most appropriate treatment:
Pre-testicular infertility — caused by hormonal problems outside the testes. The testes are normal but receive incorrect signals. Often highly treatable with hormone therapy.
Testicular infertility — the testes themselves are not producing sperm normally due to genetic factors, varicocele, infection damage, or trauma. Treatment depends on severity.
Post-testicular infertility — sperm are being produced normally but cannot be delivered due to a blockage or ejaculation problem. Often surgically correctable or manageable through sperm retrieval.
Treatment Options for Male Infertility at Dr Curo
The right treatment depends entirely on the cause identified. Here is what Dr Curo offers:
Lifestyle modification — for men with lifestyle-related causes, structured guidance on weight, diet, smoking cessation, and heat avoidance can produce significant improvement within 3 to 6 months.
Hormone therapy — for men with hormonal causes (hypogonadotropic hypogonadism), injectable or oral hormone treatments can restore sperm production in many cases sometimes dramatically.
Varicocele repair — surgical correction of varicocele through microsurgery or radiological embolisation. Improvement in sperm parameters is seen in the majority of cases within 3 to 6 months.
Infection treatment — targeted antibiotic therapy for active infections affecting the reproductive tract.
Surgical sperm retrieval — for men with azoospermia due to blockage or production failure:
- PESA — Percutaneous Epididymal Sperm Aspiration sperm aspirated from the epididymis
- TESA — Testicular Sperm Aspiration sperm aspirated directly from testicular tissue
- MicroTESE — Microsurgical Testicular Sperm Extraction the most advanced technique, used when sperm production is severely impaired, using a surgical microscope to identify and extract sperm-producing areas
IUI with processed sperm — when sperm count and motility are mildly reduced, IUI with the best washed sperm can be effective.
IVF with ICSI — for moderate to severe male infertility, a single healthy sperm is injected directly into each egg in the laboratory. This technique has transformed outcomes for men who previously had no treatment options.
Sperm donation — when no sperm can be retrieved from the testes at all, donor sperm from a screened, anonymous donor is a compassionate and effective option.
Success Rates — Can Male Infertility Be Treated?
The answer in the large majority of cases is yes male infertility is treatable, and outcomes at Dr Curo are strongly positive.
| Cause | Treatment | Success Outlook |
| Hormonal imbalance | Hormone therapy | Very good — sperm often restored |
| Varicocele | Surgical repair | Good — 50–70% see improved parameters |
| Mild-moderate low count | IUI or IVF with ICSI | Good with appropriate treatment |
| Obstructive azoospermia | Sperm retrieval + IVF/ICSI | Excellent — very high sperm retrieval rates |
| Non-obstructive azoospermia | MicroTESE + IVF/ICSI | Moderate — sperm found in 40–60% of cases |
| Lifestyle causes | Lifestyle modification | Very good — significant recovery in 3–6 months |
The key message do not assume male infertility means the end of the road. With the right diagnosis and the right treatment, the path forward exists for the vast majority of men.
Cost of Male Infertility Treatment at Dr Curo
| Treatment | Approximate Cost (India) |
| Semen analysis | ₹500 – ₹1,500 |
| Hormone blood tests | ₹1,500 – ₹3,000 |
| Scrotal ultrasound | ₹1,000 – ₹2,500 |
| Varicocele repair (surgery) | ₹40,000 – ₹80,000 |
| TESA / PESA sperm retrieval | ₹15,000 – ₹30,000 |
| MicroTESE | ₹60,000 – ₹1,20,000 |
| IVF with ICSI | ₹1,20,000 – ₹1,60,000 |
At Dr Curo, all pricing is fully transparent. You will always know exactly what you are paying for and why no hidden charges, no unexpected additions. Contact Dr Curo directly for a personalised treatment cost estimate based on your specific diagnosis.
Side Effects and Risks of Male Infertility Treatments
Lifestyle changes — no medical risks. Positive health benefits far beyond fertility.
Hormone therapy — generally well tolerated. Possible mild side effects include mood changes, acne, or fluid retention depending on the medication used.
Varicocele repair — minor surgical procedure. Risks are very low and include mild post-operative discomfort, bruising, and the rare possibility of recurrence or hydrocele formation.
TESA / PESA — minor procedures done under local anaesthesia or light sedation. Mild scrotal discomfort for 1 to 2 days is normal. Serious complications are rare.
MicroTESE — more involved microsurgical procedure under general anaesthesia. Recovery takes 2 to 3 days. Risks include temporary scrotal swelling, bruising, and in rare cases some reduction in testosterone levels post-procedure.
IVF with ICSI — risks are primarily on the female partner’s side (stimulation, egg retrieval). For the male partner, providing a sperm sample carries no medical risk.
Your Dr Curo specialist will walk you through every risk and benefit in detail before any procedure is recommended or performed.
Male Infertility and Emotional Wellbeing
The emotional impact of a male infertility diagnosis is profound and far too often ignored.
Many men receiving an abnormal semen analysis report feelings of shock, shame, inadequacy, and a deep sense of having let their partner down. Cultural expectations around masculinity make it harder for men to talk about fertility struggles openly with friends, family, or even their own partner.
At Dr Curo, we see this every day and we take it seriously. Common emotional experiences for men going through infertility diagnosis and treatment include:
- Difficulty accepting the diagnosis, especially when no symptoms were ever felt
- Withdrawal from conversations about fertility to avoid confrontation
- Guilt over the impact on their partner’s treatment journey
- Anxiety during the treatment process and waiting periods
- Relationship strain from the emotional distance that often develops
Dr Curo provides dedicated counselling for men as well as couples because the emotional health of both partners is equally important. You will find a non-judgmental, supportive environment where honest conversations are welcomed and encouraged. A diagnosis of male infertility does not define you. It is a medical finding and like most medical findings, it has a path forward.
How Long Does Treatment Take?
This depends entirely on the cause and the treatment chosen.
Lifestyle changes — improvement in sperm parameters typically seen within 3 to 6 months as it takes approximately 74 days for a new batch of sperm to be produced. Changes made today show results in the next cycle of sperm production.
Hormone therapy — response is usually seen within 3 to 6 months of starting treatment. Some cases require longer ongoing therapy.
Varicocele repair — sperm improvement typically seen within 3 to 6 months post-surgery.
Surgical sperm retrieval — sperm can be retrieved on the same day and used immediately for IVF with ICSI, or frozen for future use.
IVF with ICSI — one complete cycle takes 4 to 6 weeks. Results are known within 6 to 7 weeks of starting.
At Dr Curo, your doctor will give you a realistic treatment timeline at your very first consultation based on your specific diagnosis.
Tips to Improve Male Fertility Naturally
These evidence-based changes can meaningfully improve sperm quality at Dr Curo:
- Quit smoking immediately — one of the single most impactful things a man can do for his sperm. Improvement is measurable within 3 months
- Reduce or eliminate alcohol — even moderate drinking affects testosterone and sperm quality
- Reach and maintain a healthy weight — obesity significantly disrupts male hormone levels and sperm production
- Avoid heat to the groin — no hot baths, saunas, steam rooms, or heated seats. Switch to loose, breathable underwear
- Exercise regularly but not excessively — moderate exercise improves testosterone and overall hormone balance. Extreme endurance training can temporarily lower sperm production
- Eat a fertility-supportive diet — zinc (found in pumpkin seeds, meat, legumes), folate, vitamin C, vitamin E, and selenium all directly support sperm health
- Take a male fertility supplement — antioxidant supplements containing CoQ10, zinc, folate, and vitamin E have good evidence for improving sperm parameters
- Manage stress — chronic stress raises cortisol and suppresses testosterone. Yoga, meditation, and adequate sleep are practical tools
- Stop anabolic steroids immediately — if you are using testosterone supplements or anabolic steroids, stopping is non-negotiable before any fertility treatment
- Get tested early — do not wait 12 months if you have known risk factors. A semen analysis is simple, fast, and inexpensive
Frequently Asked Questions
Q1. Can a man with zero sperm count still have a biological child? In many cases, yes. Even when no sperm appear in the ejaculate, sperm may still be present inside the testes. Surgical retrieval techniques like TESA or MicroTESE can recover sperm directly for use in IVF with ICSI. Your Dr Curo specialist will evaluate whether retrieval is possible based on your specific diagnosis.
Q2. Does low sperm count mean low testosterone? Not necessarily. Sperm count and testosterone levels are related but not always proportional. It is entirely possible to have normal testosterone with low sperm count, or vice versa. Hormone testing at Dr Curo measures both and guides treatment accordingly.
Q3. How is a semen analysis done and is it uncomfortable? A semen sample is provided by masturbation into a sterile container either at the clinic or at home within 30 to 60 minutes of collection. It is not painful or invasive in any way. Results are typically available within 24 to 48 hours.
Q4. Can male infertility be caused by tight underwear alone? Tight underwear is a contributing factor not a sole cause in some cases of reduced sperm count due to raised scrotal temperature. Switching to looser styles is recommended but is unlikely on its own to resolve a significant sperm problem.
Q5. Does having a child previously mean male infertility cannot be the issue now? No. Male fertility can change over time. Previous fatherhood does not rule out a current sperm problem. Infections, varicocele, hormone changes, and lifestyle factors can all affect fertility between pregnancies. Always get a current semen analysis rather than assuming past fertility is still present.
Q6. Will the treatment affect my daily life or work? For most treatments hormone therapy, lifestyle changes, and even varicocele repair recovery is quick and disruption to daily life is minimal. MicroTESE requires 2 to 3 days of rest. IVF with ICSI requires the male partner only to provide a sperm sample on the day of egg retrieval no other physical demands.
Dr Curo is With You Every Step
Understanding infertility causes in men is not just medically important it is personally empowering. Knowing the cause means knowing the solution. And in male infertility, the solution exists for the vast majority of men who take the step of getting properly evaluated.
A semen analysis is not a judgment. It is information. And information is what turns a difficult journey into a navigable one.
At Dr Curo, male infertility is treated with the same expertise, sensitivity, and determination as every other aspect of fertility care. Our team of reproductive specialists, urologists, embryologists, and counsellors work together to give every man and every couple the clearest path forward.
You do not have to carry this silently. You do not have to figure it out alone. And you do not have to accept that parenthood is out of reach.











No Comment! Be the first one.